Ansar Wali clearly remembers the moment he knew he wanted to be a physician. He was a child, sitting outside a health clinic in Kabul.
A line of people spilled out from the clinic’s doors and onto the street. Rare for Afghanistan, a female doctor was making her way down the queue. It was Fatima, Ansar’s mother.
Wali recalls the empathy she spoke to patients with — and how intently she listened to what they had to say.
“My mother is my role model,” Wali—now a 29-year-old medical student at Creighton University School of Medicine in Omaha, Nebraska—says.
It was the late 1990s. With essential resources denied and medical facilities in ruins, the ruling Taliban regime had made life nearly impossible for Afghani doctors.
By 2001, Fatima couldn’t take it anymore. The decision to leave for the United States was partially due to Ansar’s mother’s wish for her children—especially her daughters—to have access to medical education.
With this regime that probably doesn’t value human life that differs from their ideology … that’s a danger. We’re losing every aspect of medicine, and who knows if they get it back.
The move cost Fatima her career and extended family, but her dream to see her child study medicine has been realized. Three out of four Wali children are involved in the medical field or about to enter it.
This summer, the Taliban regime has taken over Afghanistan once again. For the Wali family, it has felt like losing home all over again. Slowly rebuilt after the first Taliban regime, Afghanistan’s health care and medical education system again sit in extreme peril.
More than 120,000 Afghans have left home for the U.S in recent weeks. Many will be doctors or medical professional facing the same decisions Ansar’s mother made 20 years ago. Like the Wali family, the pain of leaving Afghanistan will stay with them.
“It’s almost like living two lives,” Wali, 29, says in an emotional interview. Recent weeks saw him juggle his Step I exam and clerkship preparation with the heartbreak he felt watching images from his homeland online.
“I talked to one of my friends about this. You’re here in America, you’ve put your life together, you’re a professional student, you get to dress up and drive your car – all the normal things. You perform at a high level; you’re expected to.
“This other angle is watching your homeland completely fall apart. Watching my parents, talking to them, and seeing them go through that twice—especially my Mom as a physician—it’s been very tough to just focus on school. Sometimes, I just have no motivation to get up and study.”
A doctor’s story
By 2001, Fatima was one of the last female physicians still practicing in Afghanistan.
Though one of few female students in her pre-Taliban classes, she studied at Nangarhar Medical University before opening a health clinic in Kabul. Fatima primarily cared for the city’s underserved female and children populations.
Her credentials and work ethic meant little to the Taliban, who ruled Afghanistan between 1996 and 2001. With major countries refusing to recognize the regime, international funds and resources disappeared. Given the Taliban’s fundamentalist beliefs, women’s and children’s health suffered greatly.

“As outdated notions of ‘modesty’ took precedence over medical intervention, maternal mortality soared,” Sohini Bose wrote for Observer Research Foundation—a leading Indian think-tank—in April 2020.
“Only one-third of Afghanistan’s districts had a maternal or child health clinic, and over 90 percent of all births took place at home. With poor maternal health, children suffer from birth defects, malnutrition, and preventable diseases.”
Under the ruling Taliban regime in 2001, Fatima’s hopes of her children studying medicine in Afghanistan became virtually impossible.
After arriving in America, the Wali family lived in Houston for three years before moving to Omaha in 2004. Though a highly skilled physician, America’s tricky pathway for international medical graduates meant Wali’s mother could not practice in the U.S. She took a non-medical job, often traveling out of state.
Like Fatima, hundreds of medical workers left during the last Taliban regime. They left a chronic shortage of medical professionals behind them.
Afghanistan had only 11 physicians and 18 nurses per 100,000 people in 2011. On average, the same population was serviced by less than four medical facilities.
After the U.S. military helped overthrow the Taliban in late 2001, foreign medical aid flooded into Afghanistan. India has been a leading contributor. Along with better organized Afghani government support, medical facilities grew from 500 to 2500 between 2003 and 2018.
Women’s health, antenatal and postnatal care, and pediatrics improved significantly, as did the number of practicing female doctors. Infant and child mortality dropped dramatically.
Fatima’s sacrifices paid off. Along with Ansar, two Wali siblings are now involved in medicine. Brother Isar is a respiratory therapist in Omaha, while sister Ilaha is planning on attending PA school this fall.
The human toll
By 2002—the year after the Wali family left—there were only four medical schools operating in Afghanistan. The largest school in Kabul had been partially destroyed from earlier conflict.
With laboratory facilities totally unavailable, all teaching was lectured-based. Faculty had been “decimated by emigration.” Fields such as anatomy, radiology, obstetrics and gynecology, and microbiology had no lecturers at all. Board certification was non-existent. Taliban ideology saw a generation of female med students passed over.
As a physician, your duty, your calling is to be resilient and to fight, not just for yourself – but your patients.
Though slow progress was made under the new U.S-supported Afghan government, things did improve. Between 2002 and 2011, overall student numbers grew from 1000 to 10,000, along with the establishment of 13 Afghani medical schools, in total. Female students were accepted into medical programs again.
Despite wage constraints—as recently as 2019, Afghani doctors were paid less than $200 a month in state hospitals—the pipeline produced results.
By 2016, there was nearly triple the number of physicians working in Afghanistan than 15 years before. Last year, around 41,500 Afghani medical professionals were working alongside international staff and more than 23,000 volunteer workers.
How many have escaped the country in recent weeks is unknown, but numbers are likely to be significant. Along with international physicians who have left, Wali says their absence will be keenly felt.
“We learn best from our colleagues, from our best attendings that we get to follow on our rotations,” Wali says.
“Not having people who can provide that for those citizens [who wish to become doctors] and people who are in medicine, in Kabul and around Afghanistan, that hurts. Who are [they] going to look up to?”
Beyond the initial wave of Afghani refugees, a repeat of the medical brain of the late 1990s is inevitable. Many Afghani med students—like Salgy Baran, the nation’s top high school graduate and aspiring physician—face a tough road ahead if they wish to continue studying. Like Ansar’s mother, large numbers will surely leave medicine.
“The most difficult thing is knowing how hard it is [to] get into med school as an immigrant – and now others who are refugees,” Ansar says, of those that make a new home in the States.
“That road for them to get to where they want to be, not necessarily med school, I’ve reflected a ton on. It hurts every time I think about that because it takes so damn long to even get in front of an admissions committee, let alone an undergraduate medical advisor.”
‘… a dysfunctional or non-functional administration.’
There is some hope the new Taliban regime will be less like the last one when it comes to health care.
“In the areas they dominate,” Bose wrote last year, “the Taliban has created a parallel system of governance through governing commissions responsible for administrative affairs, including health.
“Currently, healthcare in Taliban areas is a hybrid of non-government organizations (NGOs) and state-provided services. The Taliban monitors clinics, checks staff attendance, and inspects equipment and medicine stocks.
“It has also been pressuring NGOs to expand healthcare access in rural areas and improve the quality of services.”
In early August, Filipe Ribeiro, the Afghanistan representative for Doctors Without Borders, told NPR that they had been in touch with Taliban leadership across the country throughout the “transition.” Some Doctors Without Borders medical staff have fled the country, but most have now returned to work.
“For the time being, we can work without a problem from the other side,” Ribeiro says. “As I said, the transition is ongoing. The [Taliban] administration is not yet fully at work. Let’s see how it goes.”
Despite the hope, the warning signs are also there. In 2019, the Taliban “shut down 42 health facilities in the central province of Maidan Warduk, attacked hospitals, and held patients as hostages.”
Dozens of Indian medical staff have been murdered, while its diplomatic outposts were attacked multiple times. India’s continuing aid is far from certain. A complete withdrawal of its assistance would be disastrous for the Afghani health care system.
The Taliban’s recently announced national cabinet has prompted fears of a worst-case scenario: a return to the fundamentalist restrictions of the late 1990s and a second disappearance of international medical aid. Any gains in women’s and child’s health would vanish.

“When influence moves out, when power moves out, we’re kind of leaving it up for grabs,” Wali says.
“With this regime that probably doesn’t value human life that differs from their ideology … that’s a danger. We’re losing every aspect of medicine, and who knows if they get it back.”
A lack of action will soon show its cost. Though it has recently emerged from the third wave of Covid-19 infection, a larger Delta outbreak would further paralyze Afghanistan’s struggling medical network.
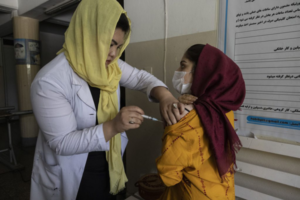
Only 2.6% of its total population is fully vaccinated so far. Since the new regime took over, there has been an 80% drop in vaccinations. The Taliban’s stance on Covid-19 vaccinations is still unclear.
While still operating, Doctors Without Borders says many of their clinics have become isolated due to a shutdown of domestic air travel. Supply chain issues are being felt by both state or internationally-run facilities.
“How are we going to get the medicines in? Or get people in and out, or travel around the country?” Ribeiro says.
“Just doing things as basic as [getting] a visa, it’s almost impossible for the time being because there is a dysfunctional or non-functional administration.”
‘I’m not going to leave my people behind’
More than 20 years after he sat outside her health clinic, Wali now knows the risks his mother had to take to do her job.
He understands why Fatima’s passion for medicine forced their family to leave home—and how that decision helped lead him to the very same vocation.
“When we talk about being physicians, it’s not about being burnt out,” Wali says.
“It’s about providing the care for patients that need it in a way that’s most appropriate. Getting a glimpse of that [as a child] … it makes you think.”
How are we going to get the medicines in? Or get people in and out, or travel around the country?
Though his heart breaks for his homeland, Wali is also determined to help fellow Afghani in need.
He has been in touch with the Afghan embassy in Washington DC to build links with young Afghani students hoping to study medicine in the U.S. and says he’d leap at the chance to return as a practicing physician one day.
Despite the likelihood of healthcare and medical education in Afghanistan being set back decades, Wali has full confidence in those doctors who remain in Afghanistan. After all, he has seen it in action.
“As a physician, your duty, your calling is to be resilient and to fight, not just for yourself – but your patients,” Wali says.
“There’s something about those countries in Central Asia. They are prideful, resilient, and [their approach is] ‘I’m not going to leave my people behind.’ There will be individuals who take that chance.
“They will see that as an opportunity to be a leader in a different way, continue to practice medicine, and move forward to not only provide care but help future students into medicine.”


